Understanding Field Loss
Presented on Friday 2 November 2007
Neurological Causes of Visual Field Loss: Epilepsy (surgical treatment), Cerebral palsy, PVL, Tumour, Stroke.
Dr Andrew Blaikie, Consultant Ophthalmologist, NHS Fife
Cerebral Palsy
- Motor impairment due to some kind of brain injury
- Often unknown
- Often associated with other impairments
- Not cause of visual impairment
- It's an associated symptom
Spastic Cerebral Palsy
Children with this type may find their muscles becoming very stiff and weak, especially under effort. This can affect the way they move.
Athetoid Cerebral Palsy
Children with this type of cerebral palsy often lose control of their posture. They may also tend to make unwanted movements.
Ataxic Cerebral Palsy
Children with this type of cerebral palsy usually have problems with balance. They may also have shaky hand movements and irregular speech.
Cerebral Palsy
- Visual Acuity
- Visual Field
- Eye Movements
- CVI
- Refractive Errors
- Accommodation

Lower field defect

May not be completely lost

Cerebral Palsy + PVL
Patient with spastic diplegia form of CP complaining of difficulty with tasks involving lower field.
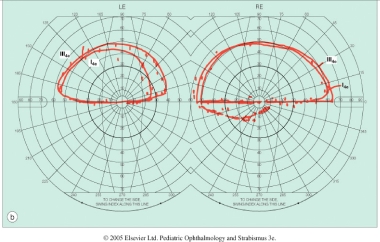
Periventricular Leucomalacia PVL
Brain Damage in Premature Babies
- Hypoxia
- Hypo-perfusion
- Leads to brain injury of Periventricular White Matter
- Spastic Diplegia
- Visual Impairment

Cerebral Visual Impairment
Two streams of visual information in the brain
- The ‘Where’ stream
Fast reflex unconscious information to act upon - The ‘What’ stream
Slower conscious recognition of world

Simultanagnosia
- Inability to deal with complex scenes also known as simultanagnosia
- Functionally visual field becomes small
- Poor attention and easily distracted
- Sticky fixation
Epilepsy - Hemispherectomy
- Used in intractable seizures
- Surgical removal of portions of the non functioning hemisphere combined with splitting the corpus callosum.
- This is the channel which allows signals to cross from one side to the other.
- Stops the seizure starting at one hemisphere and travelling to the other
- Mainly removes portions of the temporal lobe which can cause quadrantopias or removal of occipital lobe can results in homonymous hemianopia.
Homonymous hemianopia


However, in children some functional field can still result despite removal of occipital (site of the visual cortex)
Thought to be mediated by higher cortical areas or subconscious visual pathways via the midbrain/brainstem (Werth, Reinhard , 2006)
Epilepsy
- Not all children with epilepsy will have visual field loss
- Usually it is the treatment (both surgical and medical) for epilepsy rather than the condition itself which gives rise to field defects.
Infantile Spasms
- Fitting from early age
- Difficult to control
- Delays development
- Often associated with structural brain problems
Medication
- VIGABATRIN – anticonvulsant drug
- Used in the treatment of generalized seizures and infantile spasms
- Field defects noted after approx 1 year treatment
- Prevalance of between 42% (Wohltab, G et al., 1999) and 71% reported (Russell Eggitt, IM et al 2000)
Vigabatrin
- Atrophy of the retinal nerve fibre layer sparing macular area
- Generalised constriction of visual field
- May not be reversible (Hardusa P et al (2000)


Tumours
- Craniopharyngioma
- Pituitary
- Glioma
- Menigioma
Tumours
- Approximately 50% of childhood intracranial tumours will have visual symptoms
- Whether Benign or Malignant
- Tumours create pressure on the signals within the visual pathway
- Direct – within the visual pathway
- Indirect – by raising the intracranial pressure – (although unlikley to be aware of field defect from enlarged blind spot)
Craniopharyngioma

Arises from stalk of pituitary
- Presses on chiasm from behind and above
- Young patients present with pituitary problems or hydrocephalus
- Older complain of visual disturbance
Pituitary Tumours

Craniopharyngioma and Pituitary Tumour
- Field loss - bitemporal hemianopia or (quadrantopia in early stages)
- CP compresses chiasm from above PT compresses from below.
- Chiasmal lesion only – will give rise to a different field defect in each eye that is, loss of right field in right eye and left field in the left eye.

Neurofibromatosis
Gliomas and Meningiomas
Neurofibromatosis
- Type 1 - von Recklinghausen or Peripheral
- Type 2 - Central
Both have: - Typical marks on the skin
- An increased risk of developing tumours

Causes of VI
- Tumours
Optic Nerve Glioma (type 1)
Optic Nerve Mengioma (type 2) - Glaucoma (type 1)
- Cataract (type 2)


Hydrocephalus
- Imbalance in the production and drainage of cerebral spinal fluid (CSF)
- Fluid reservoirs (ventricles) in brain expand

Causes of Hydrocephalus
Multiple
- A-C malformation
- Brain tumour
- Neonatal brain haemorrhage
- Infection
- Unknown
How does Hydrocephalus affect vision?
- Optic Atrophy
- Chiasmal Compression
- Occipital Lobe Damage
- Eye Movement Problems
- Squint
- Nystagmus
- Supranuclear disorders (setting sun)
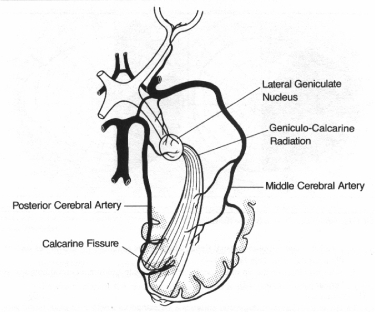
Stroke
- Does occur in children caused by infarct or haemorrhage
- Visual field defects caused by involvement of posterior cerebral artery
- Often secondary to another condition –
heart problem
sickle cell anaemia
tumour
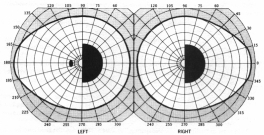
Type of field loss - hemianopia
Left hemianopia arising from lesion Right occipital lobe
Central vision spared

Separate artery supplies neurons responsible for central vision

Central Homonymous Hemianopia
Lesion on left side of brain
Spared Peripheral field
Summary
- Ocular and Brain causes of field loss
- Highly variable conditions
- Some progressive
- Some stable
- Generally untreatable
Helpful to identify field loss to aid development of habilitative strategies.